To combat a respiratory infection, the physique needs a two-pronged assault. Very first, it sends immune cells to the scene to destroy the pathogen. Then the defense method need to keep all those first responders from spiraling out of control. If this endeavor at “peacekeeping” fails, a operate-of-the-mill fever and cough can escalate to a existence-threatening illness—which occurred to the tens of thousands of COVID-19 patients who have succumbed to the world pandemic triggered by the SARS-CoV-2 virus.
For the most part, macrophages—the large immune cells that consume pathogens—are first responders. In the lungs of mice contaminated with viral influenza, nonetheless, a compact subset of these white blood cells does just the reverse: They suppress excessive swelling, researchers report now in the journal Science Immunology. These peacekeeping macrophages also reside in human lungs, suggesting they “might be extremely vital to enable COVID-19 patients resist swelling and it’s possible survive,” states immunologist Yufang Shi of the Very first Affiliated Clinic of Soochow College in China. The healthcare facility despatched staff and provides to the nation’s town of Wuhan, but Shi was not concerned in the new analyze.
The investigate began 7 yrs ago, when Kamal Khanna, an immunologist now at NYU Langone Health, noticed anything he discovered to be gorgeous. At the time, his lab was finding out a comparable group of macrophages—not in the lungs but in the spleen, a blood-filtering organ in the lymphatic method. On stained mouse tissue considered beneath a microscope, the macrophages shaped blue rings about immune-cell-abundant spots of the spleen. “They seemed like nebulas,” Khanna states.
And these cells were being not just visually amazing. When the researchers depleted the macrophages working with a clever genetic system, the mice died just two days just after becoming contaminated with compact quantities of Listeria germs they would commonly obvious. Yet another observation was also placing: although other immune cells packed infection-battling zones in the spleen, this group of macrophages stayed place. “And we imagined, This compartmentalization has to be present in [nonimmune] organs as well,” Khanna states. The spleen findings, posted in 2017, laid the groundwork for the new analysis in lungs.
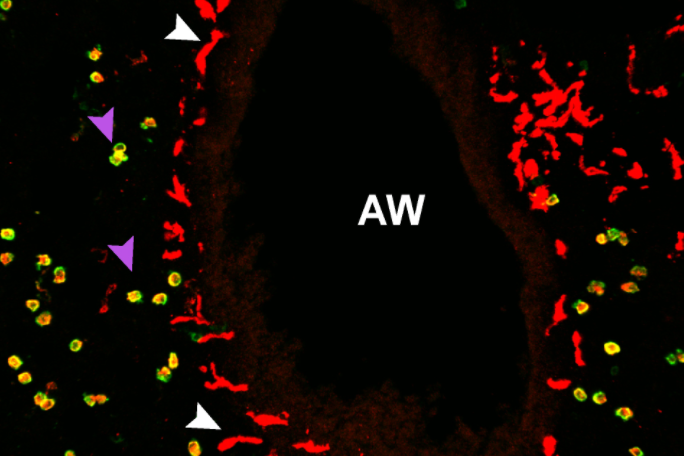
In this complicated organ, the huge vast majority of macrophages are living in very small air sacs termed alveoli. But when the researchers examined the lung tissue beneath the microscope, they saw a significantly smaller populace that was starkly diverse. Contrary to alveolar macrophages (AMs), which are large and round, the rarer macrophages are elongated with sprawling arms — and they are not discovered in alveoli. Called nerve- and airway-connected macrophages, or NAMs, these freshly determined cells congregate at airways and interact with bordering nerves. “The complete airway department gets lit up with these macrophages,” Khanna states.
In a different set of experiments, his group depleted mice of AMs or NAMs and then contaminated these animals and typical mice with an influenza virus and when compared the amount of virus in the teams. These experiments disclosed a division of labor: AMs enable to combat the virus although NAMs keep the peace and reduce tissue injury.
This form of differentiation could verify vital for planning therapies targeted at swelling, which is a big difficulty in COVID-19, states Mallar Bhattacharya, a macrophage biologist at the College of California, San Francisco, who was not concerned with the investigate but calls it a “clever application of novel instruments for deletion of certain macrophage subsets.”
NAM-depleted mice created bigger amounts of a number of inflammatory molecules, which include 1 termed IL-six that is concerned in so-termed “cytokine storms” witnessed in some patients with significant COVID-19. In a modern analyze of 191 folks dealt with for the disease in Wuhan, blood IL-six amounts were being elevated in patients who died of it, when compared with survivors. Scientific trials are now assessing IL-6–blocking antibodies—drugs that are used to address rheumatoid arthritis—in COVID-19 patients.
The new analyze did not deal with how the intertwining of NAMs with nerves relates to the functionality of these immune cells. Khanna hopes to get insight in upcoming mouse experiments by depleting NAMs and examining the well being of bordering nerves or by examining how the airway nerves are affected for the duration of diverse styles of infections. The anxious-immune link is intriguing in light-weight of modern investigate suggesting that chemical cross chat involving gut macrophages and nerve fibers can control peristalsis, the approach that moves foods via the digestive tract.
A more urgent question is whether NAMs are concerned in COVID-19. Toward that end, Khanna is doing the job with NYU Langone Health to acquire clean lung tissue from folks who died of the disease—but undertaking so is logistically hard and probably risky. An even greater problem for now, in light-weight of New York City’s soaring selection of situations, is that “basically, our lab is shut down,” Khanna states.
Study more about the coronavirus outbreak here.
