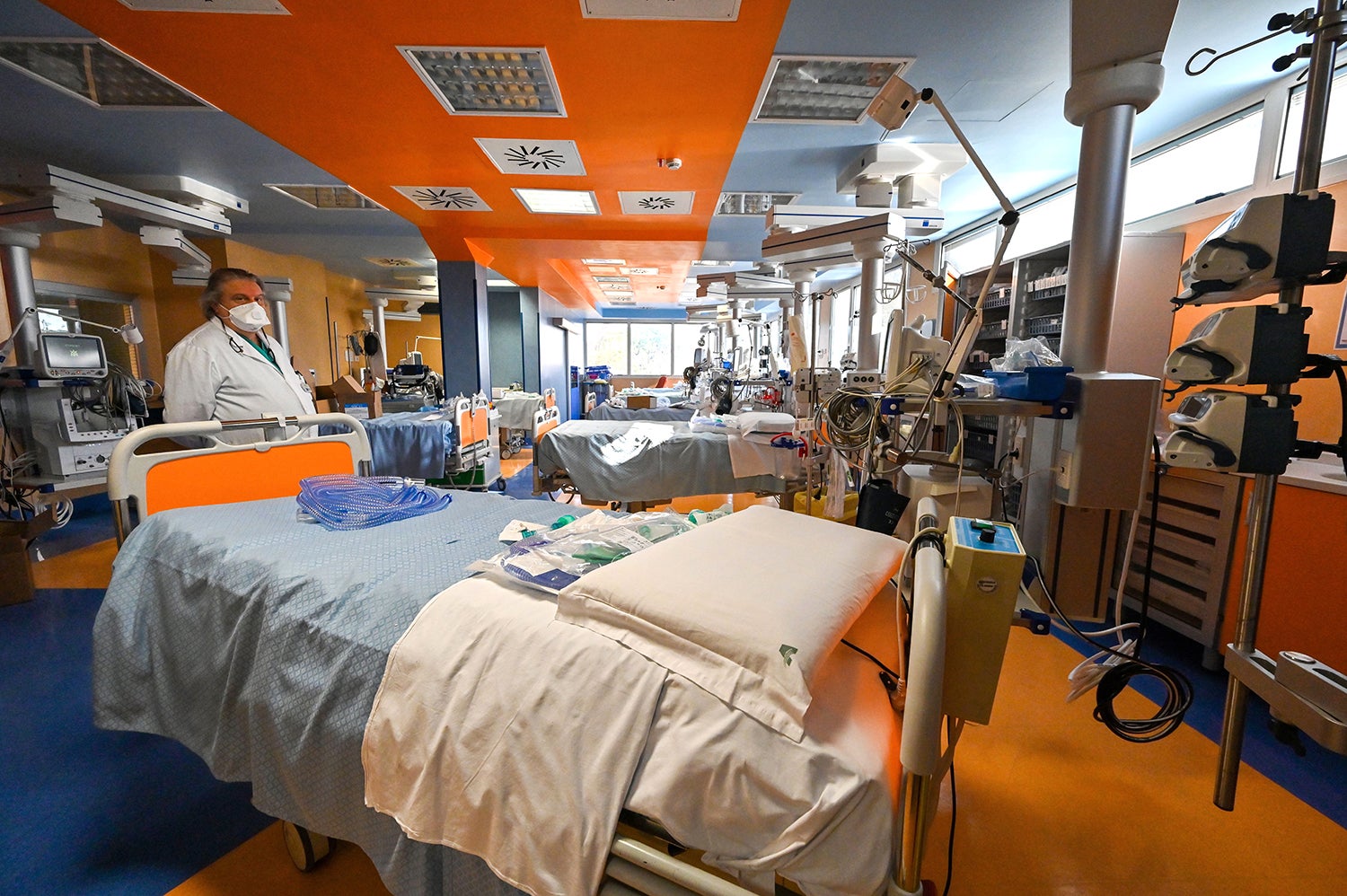
People with COVID-19 have inundated hospitals in Italy, forcing medical practitioners to make agonizing selections about who need to receive lifesaving treatment. Affected individual surges could shortly demand from customers distressing triage selections in U.S. intensive treatment models (ICUs), as well. As of Thursday, there had been extra than 13,000 confirmed cases in the U.S., and the nationwide death toll had risen to one hundred seventy five.
In February a examine in Operations Investigate employed mathematical modeling to determine which variety of triage policy could be helpful in an ICU in the course of this sort of a surge. The paper analyzed conditions in which sufferers could be queued for admission to a hypothetical ICU with confined beds or transferred to a typical ward as their condition changed. The aim was to find a heuristic, or rule of thumb, for clinicians that minimized the typical mortality level of all sufferers in excess of time, which is the aim of triage in the authentic world.
“A whole lot of periods, clinical pros are truly targeted on generating this one decision for the patient who is proper in entrance of them,” claims Laura Albert, a units engineer at the College of Wisconsin–Madison, who was not included in the examine. “It’s truly challenging when they have to inquire the patient to wait around for the reason that that will help save quite a few extra life throughout the system. These heuristics are truly valuable for service vendors, for the reason that otherwise it is so challenging for them to make that simply call in the moment.”
Utilizing laptop or computer simulations, the researchers utilized a heuristic that decided who need to be admitted to an ICU bed by estimating how considerably every patient’s possibilities of survival increased by becoming there and then dividing the figure by the selection of times that individual would in all probability have to have to stay. People today whose ratio was maximum had been prioritized. The researchers also examined how the heuristic labored when added patient health and fitness situations had been extra.
The examine in comparison the heuristic’s collective mortality prices with people of attainable triage eventualities. A single policy supplied beds on a first come, very first served foundation. An additional discharged sufferers who had been the least likely to be even worse off in a typical ward to make area for new ones. A third technique randomly discharged people from the ICU when new sufferers arrived.
All round, the ratio heuristic prioritized sufferers who had been predicted to receive the maximum benefit for each every day they occupied an ICU bed. Study co-author Nilay Argon, an functions researcher at the College of North Carolina at Chapel Hill, claims it was especially valuable when an individual’s state improved or worsened in the course of his or her stay. “As shortly as they transform state, then their triage need to be utilized once again,” Argon claims. Earlier functions products of triage selections in ICUs have not considered a patient’s condition getting distinct, she adds.
A very first appear, very first served technique employed in one clinic in Wuhan, China, when the coronavirus began to spread might not have been the ideal method. Shu-Yuan Xiao, a pathologist at the College of Chicago, was in Wuhan at that time and observed how health and fitness treatment personnel responded. He even assisted them. “The hospitals had been confused,” Xiao claims. “They just didn’t have that quite a few ICUs, and the ICUs had a very first appear, very first served” policy in the beginning, which might have contributed to the original significant mortality prices in the city.
“Health treatment is only as great as the assets that we have for it, and the assets out there [for one patient] are basically a function of how you deal with other sufferers,” Albert claims. “You cannot generally make these treatment method selections in isolation. And we truly see this when there’s a large patient surge.”
Edieal Pinker, an functions researcher at Yale College, claims reserving a bed for seriously significant patients—a follow referred to as “idling”—when much less significant folks are ready brings still one more layer of complexity to triage. “Once you have tied up that bed, you’re blocking any person,” he claims. “It’s a challenging decision to make, for the reason that you’re telling a patient who’s in entrance of you now [that] they cannot have this. That is challenging for people to do, so you have to have pointers and self-control.” The new examine only addressed nonidling insurance policies.
Comparable to what the new product indicated, when a patient with a minimal probability of recovery is tying up an ICU bed for quite a few times, and multiple other sufferers could be stabilized in that bed, Pinker claims, clinicians will have to make the decision to transfer that patient to palliative treatment. “The threat, however, when you transfer infectious COVID-19 sufferers, is that you have to have a spot to transfer them in which you’re not likely to finish up spreading the virus even further more,” he adds.
Versions are not necessarily the last remedy, claims Jennifer Horney, an epidemiologist at the College of Delaware’s Catastrophe Investigate Middle. She cautions that designed-in assumptions might not translate to authentic-world eventualities. “I assume that we can take into consideration [products] as part of a planning resource,” she claims. But “it’s critical to be even handed when utilizing information from modeling to test and predict exactly what is actually likely to come about in a authentic-lifetime scenario.” Horney claims that “after-event” scientific tests that accumulate information from health and fitness treatment amenities next a authentic outbreak, this sort of as the 2009 H1N1 pandemic, and use them to predict what would come about in a related party, might be preferable to products that make assumptions that might or might not play out.
Without a doubt, it might be as well early for hospitals to use the new study’s heuristic to a COVID-19 patient surge. A single trouble is a deficiency of information on the survivability prices of the illness, claims Scott Levin, a biomedical engineer at the Johns Hopkins Faculty of Medication, who co-built an electronic triage system for Johns Hopkins, a machine-finding out program that makes use of health and fitness document information to assist categorize emergency area sufferers. “We really do not truly have a whole lot of historic information about who’s likely to benefit from an intensive treatment unit,” he claims. As information accumulates, Levin claims, up to date products can produce triage tips that are extra attuned to what is going on with COVID-19.
Without having sturdy survivability information, adaptability will be crucial to working with a coronavirus patient surge, claims Pinar Keskinocak, a units engineer at the Georgia Institute of Technology. She claims it is critical for health and fitness system directors and policy makers to assume outdoors the box about how to modify workflow and procedures.
A single case in point comes from Demetrios Kyriacou, a physician at Northwestern Memorial Hospital’s emergency department—a entrance line for triage that has about a hundred beds. Kyriacou claims the hospital’s catastrophe committee has mentioned expanding the triage place into other pieces of the facility, even together with an ambulance bay, need to the have to have arise. “If we would have intervened before in conditions of isolating people who are ill, I assume we would have a considerably much less problematic epidemic likely on in this region,” he claims.
